Hypermobility and physiotherapy
What is hypermobility

Hypermobility is an umbrella term that covers several conditions and syndromes. Though the causes are different, the common denominator is the same - overly flexible joints. Hypermobile joint is the joint that can bend beyond the typical range of movement in one or several planes.
Hypermobility is common, estimating from 1 to 3 in 10 people, however women, children and people of Asian descent are affected more often. Some occupations statistically have more hypermobile individuals, e.g. dancers, gymnasts, athletes and musicians, however it’s not a causal but selective effect as those with hypermobility are likely to perform better.
Symptoms: not just flexible.
Most hypermobile people are asymptomatic and don’t have any complaints. For a smaller proportion (about 10%) of hypermobile people however, the hypermobility is symptomatic bringing wide and seeming unrelated array of symptoms:
- Joint instability and hyper-extension, sprains, strains, subluxations, and/or dislocations
- Chronic fatigue
- Poor proprioception which often manifesting as clumsiness, poor fine motor skills like messy handwriting
- Autonomic dysfunction Including postural tachycardia syndrome (e.g. dizziness, fainting, light-headedness, difficulty regulating temperature)
- Pain or excessive fatigue after routine sport or exercise
- Stomach and digestive problems (like reflux and slow stomach emptying)
- Bowel problems, e.g. irritable bowel or food allergies and intolerances
- Adoption of end-range postures e.g. slouching, sway back.
- Anxiety and/or depression
- Poor wound healing
- Long term (persistent) pain, fibromyalgia, non-specific low back or hip pain.
- Stretchy or soft skin
Symptoms vary a lot from person to person, and also with time. Injuries, illnesses, physical or life stressors can often tip scale for the body from compensated and coping into decompensation and “not coping” state where new symptoms appear, or existing symptoms get worse.
Types
There are four major groups of conditions leading to hypermobility:
- Specific genetic (heritable) conditions affecting the elasticity of the connective tissue and collagen in the body, such as Ehlers-Danlos syndromes, Marfan syndrome, Stickler syndrome, osteogenesis imperfecta and others.
- Loose joints, ligaments or poor muscle tone without a specific identifiable connective tissue disorder. Commonly termed as Joint Hypermobility Syndrome or Hypermobility Spectrum Disorder. This is the diagnosis of exclusion where all other specific causes have been ruled out.
- Injury- or repeated stretching/training-related hypermobility, local to single joint or multiple joints.
- Other conditions where hypermobility is a secondary effect, e.g. Down’s syndrome, cerebral palsy and others.
Group 1 requires medical investigation and testing for specific diagnosis. Majority of hypermobile people though will fall into groups 2 and 3 (if group 1 is excluded) based on following criteria:
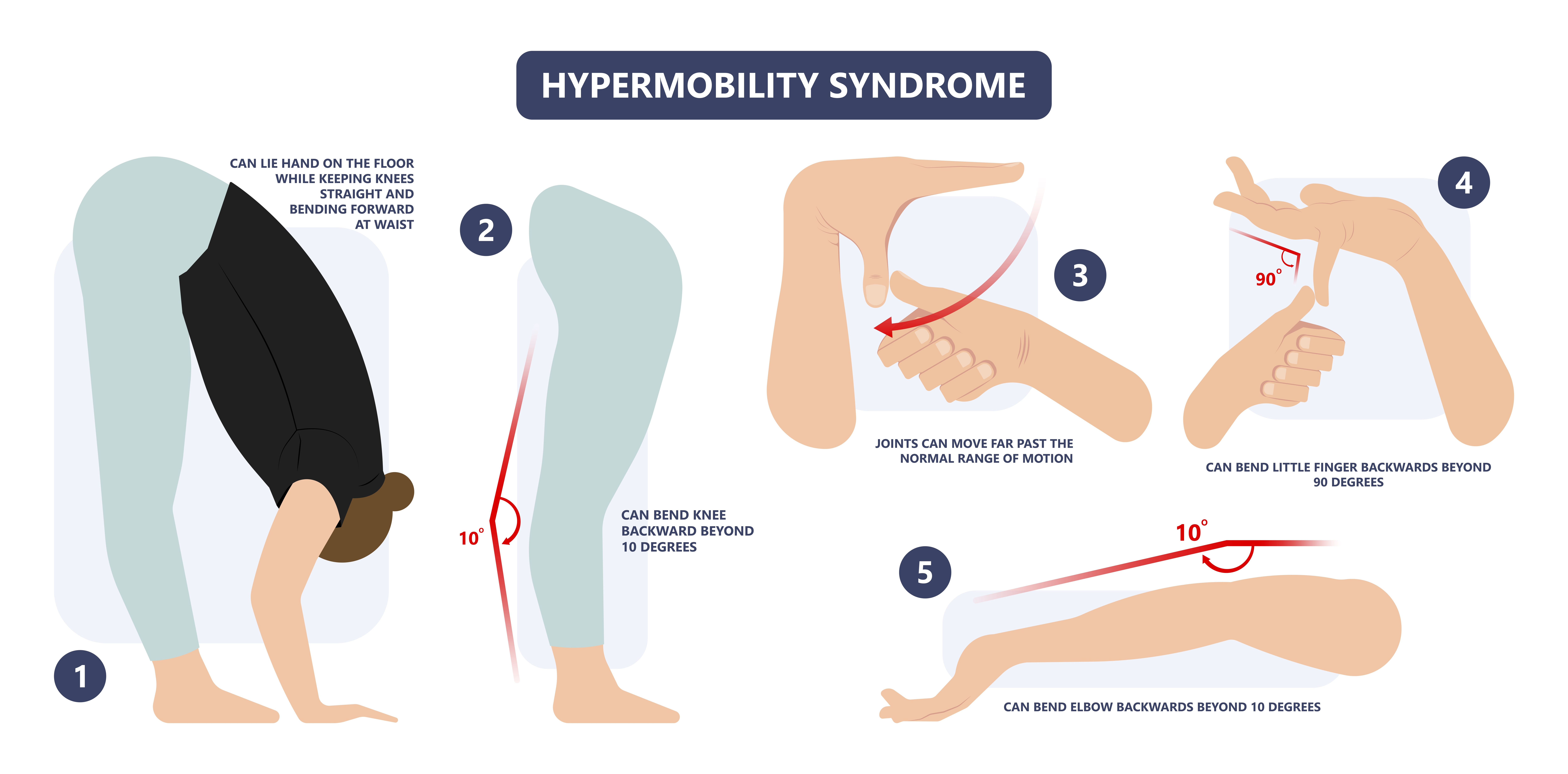
- Generalised hypermobility spectrum disorder (gHSD): is assessed using the Beighton score (see picture), along with secondary musculo-skeletal manifestations (listed above in Symptoms)
- Peripheral hypermobility spectrum disorder (pHSD): Joint hypermobility of the hands and feet, and 1 or more musculoskeletal manifestation (listed above in Symptoms)
- Localised hypermobility spectrum disorder (lHSD): A single joint or group of joints is hypermobile, with one or more secondary musculoskeletal manifestations (listed above in Symptoms)
- Historical hypermobility spectrum disorder (hHSD): Symptoms of gHSD are reported, but the individual is no longer as hypermobile as joints have stiffened with age, injury, or surgery etc.
- Asymptomatic hypermobility: hypermobility is present, but without symptoms.
Key Management
Although there are key differences in the causes of hypermobility, the management approach is similar for majority of the presentations. Physiotherapy plays a pivotal role in the hypermobility management for a symptomatic patient as the practitioner can bring together musculoskeletal, functional and psycho-social goals and methods into the management plan.
Treatment goals will vary from person to person; however the exercise therapy is key addressing the majority of the hypermobility-associated problems:
- Improving strength and postural stability therefore stabilising the joints posturally or through movement
- Reducing the impact and risk of injuries
- Modulating nervous system with movement thus reducing anxiety and autonomic nervous system symptoms
- Reducing sensitivity to movement and physical load
- Improving mood
- Improving fatigue and energy levels
Other modalities used in hypermobility treatment include manual therapy, load management, relaxation techniques, education and advice to address beliefs and fear.
Management of hypermobility is ongoing and often requires the changes in the lifestyle to incorporate the exercise.
Our physiotherapists are able to assess your body’s needs and build comprehensive rehabilitation plan to help you get your symptoms under control and reduce their impact on your life, as well as achieve your functional goals and improve your physical function.
.svg)

)-(Posters-(Portrait))-(Instagram-Post-(45)).png)



